Value-Based Care is a healthcare delivery model that rewards quality, outcomes, and cost efficiency rather than volume of services. Success depends on data-driven insights, proactive care, and strong collaboration between providers and payers.
Registration is open for the 2026 User Conference! > Register now
Value-Based Care Reporting
Azara empowers organizations to achieve better outcomes for their patients through a proven, scalable technology platform.
Azara delivers timely, actionable clinical insights to care teams that facilitate collaboration with health plans and other value-based care enablers.
This enables healthcare organizations to work hand-in-hand with health plans on critical initiatives like engaging attributed members in preventive care, improving clinical quality, capturing risk adjustment factors, and driving performance improvement. By equipping providers with up-to-date actionable information and streamlining risk gap closure and the sharing of supplemental data, Azara fosters a collaborative environment where all stakeholders can work together to monitor, track, and improve quality, cost, and utilization outcomes for the entire patient population.
Azara seamlessly integrates health-plan provided data, such as rosters and claims from multiple plans, within existing workflows. This unified dataset enables member-focused programs to optimize quality measures, close risk and care gaps, and precisely identify and target high-risk patients through risk stratification – all within the unified Azara DRVS platform.
Azara DRVS further supports value-based care success with an experienced Clinical Transformation team and a comprehensive library of over 600 measures – including over 50 certified HEDIS® measures, CMS eCQM measures used for MSSP, MCP, & PCF programs, and a broad range of other clinical quality measures, covering all health plan members.
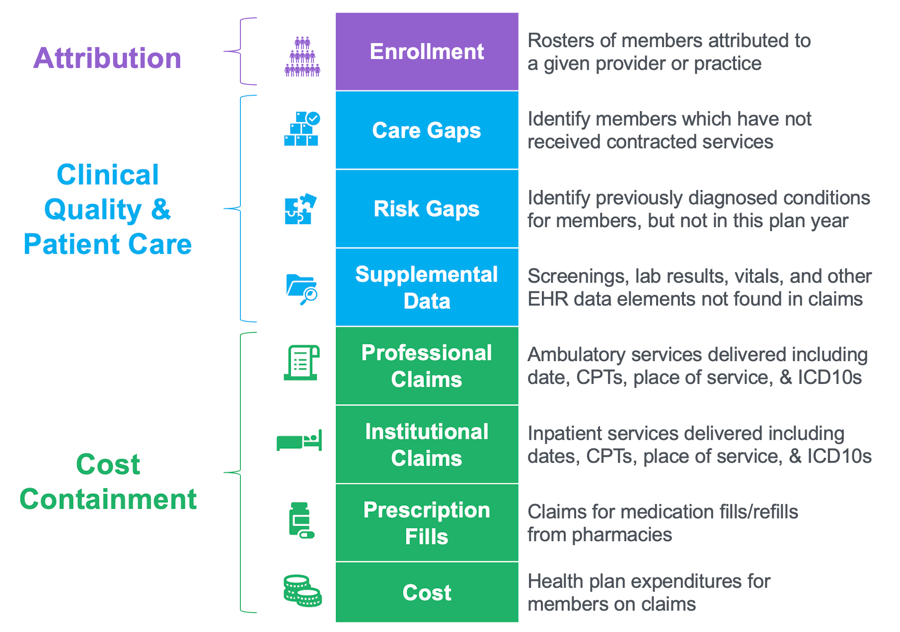

Organizations use Azara solutions to engage with health plans and members – improving care by enabling providers to:
Unify member insights by aggregating and standardizing supplemental data directly from health plans – empowering care teams with a comprehensive and timely understanding of patients' conditions and risk factors.
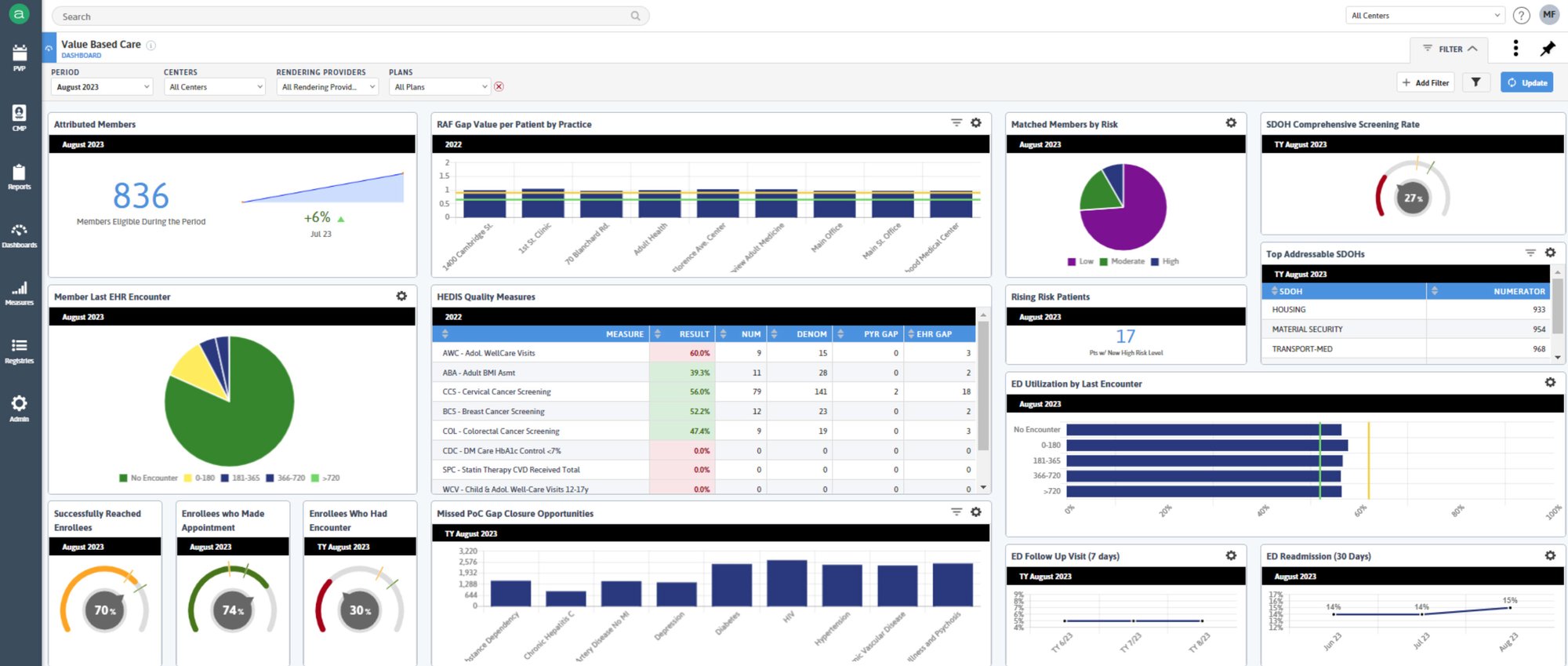

Plug-In Plan Care Gaps surfaces the status of care gaps as reported in the Care Gap Reconciliation (CGR) Report for a given patient, based on records found in the EHR and received from the Payer. This new section can help prompt care team members to document, conduct outreach, and provide the care needed to close gaps and improve measure performance.


Access real-time risk stratification to continuously identify and address potential member health issues.
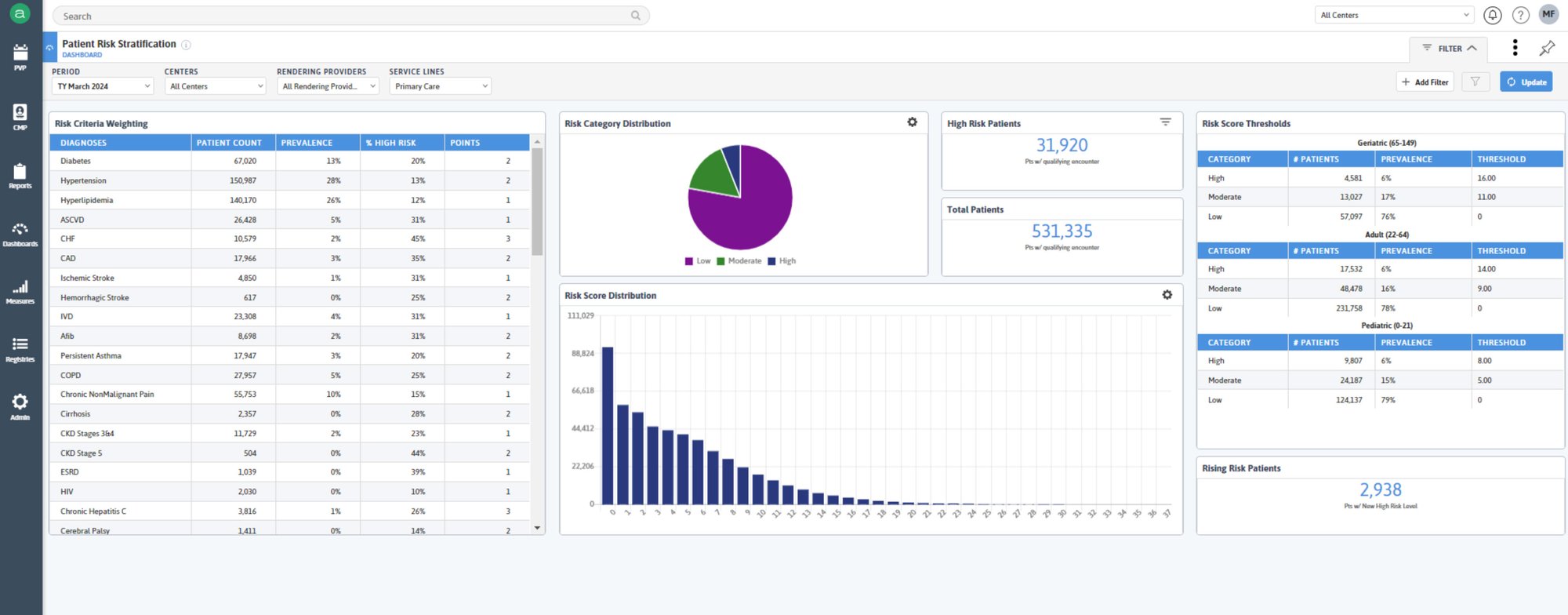

Leverage expanded clinical insights, including social determinants of health (SDOH) and demographics to optimize HEDIS measure performance and facilitate risk recapture.
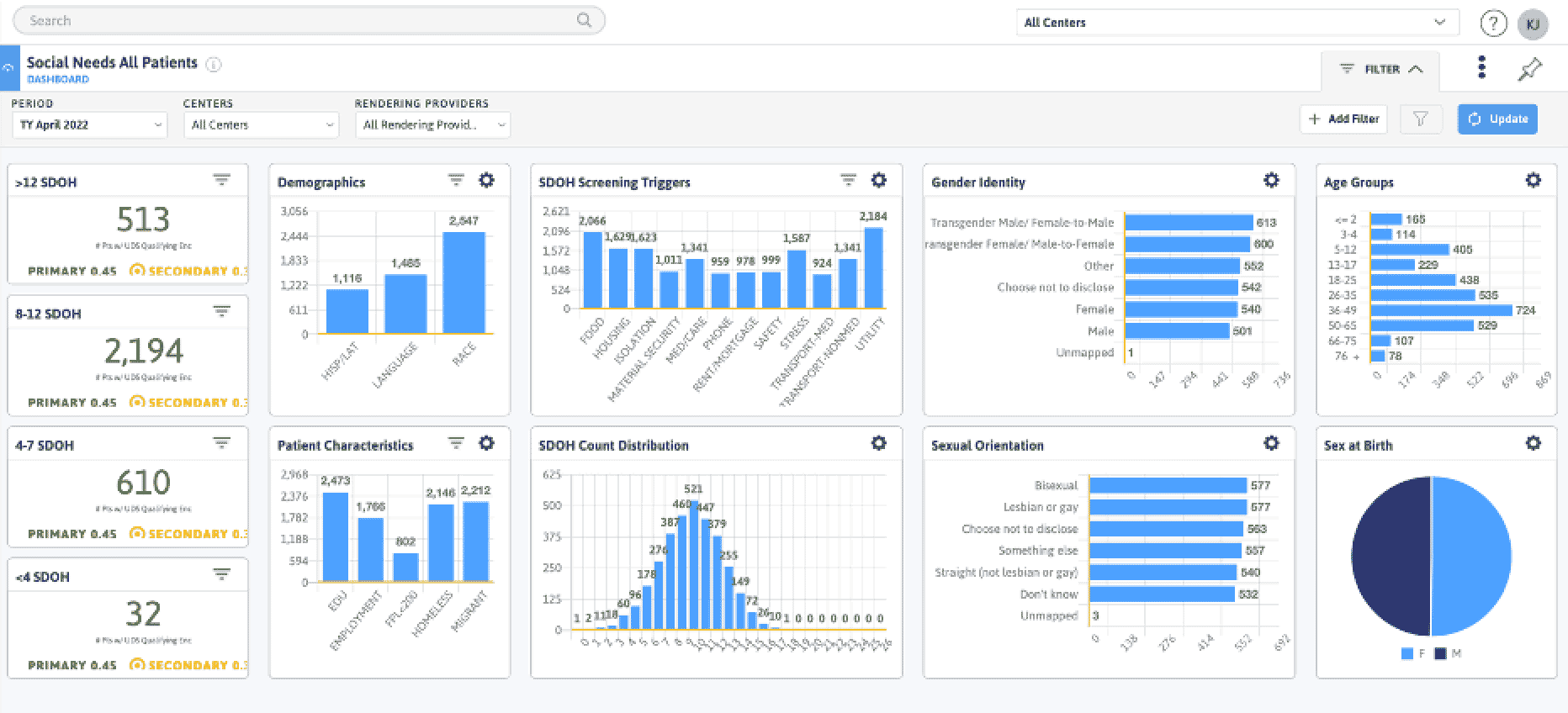

Gain granular insights into cost and utilization drivers throughout the network, enabling targeted interventions to optimize performance at the network, practice, and provider levels.
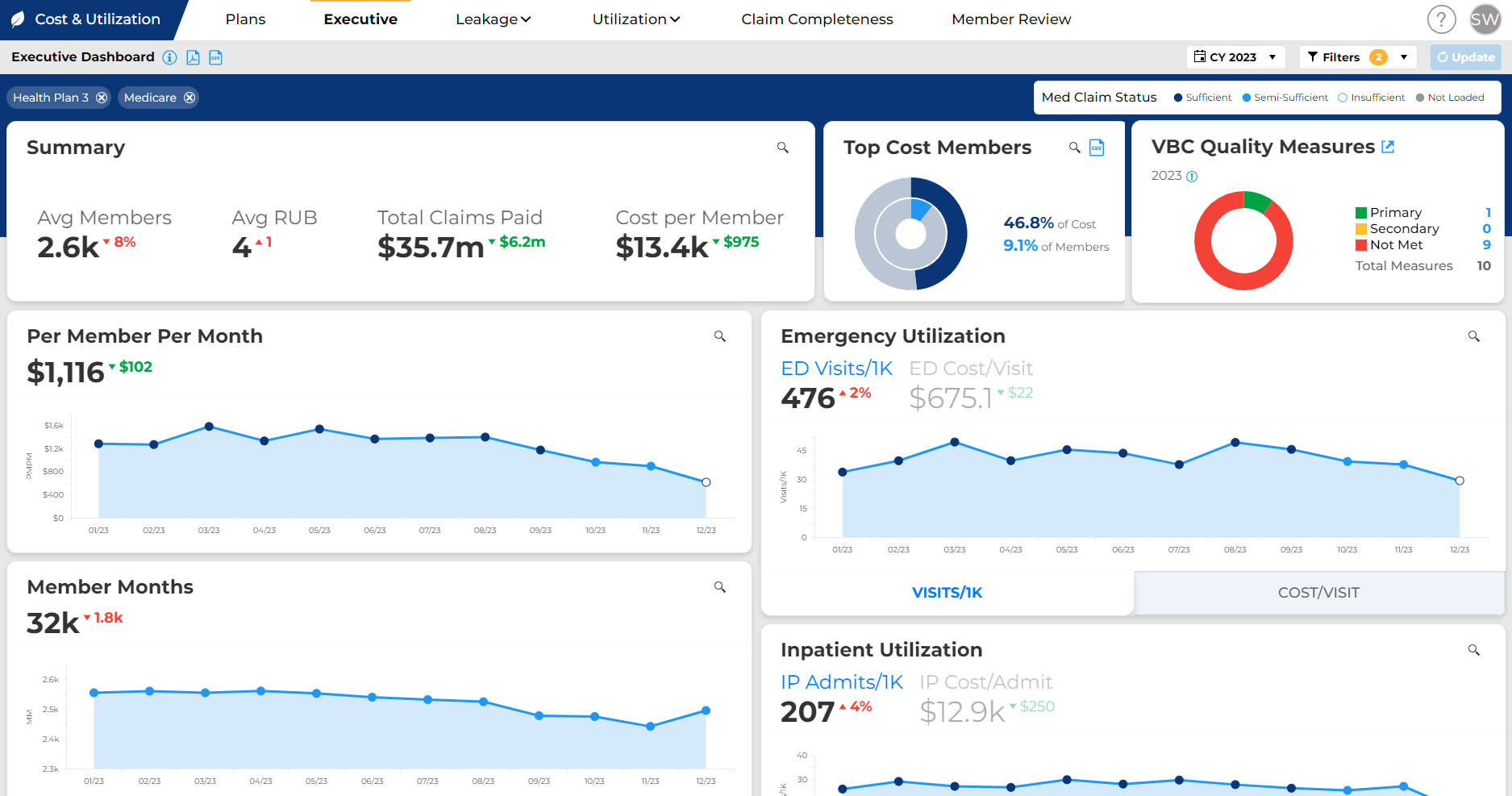


Azara DRVS empowers users to navigate the complexities of value-based care with a highly configurable and feature-rich platform, which includes:
Intuitive Dashboards
Uncover performance insights at a glance. Intuitive dashboards offer a clear, high-level view and empower users to drill down seamlessly into specific data sets for deeper analysis.
Innovative Dynamic Cohorts
Identify members who need specific services and automatically align members to relevant programs or interventions based on daily updates to their health data.
Data Activation
Equip health plan teams with actionable clinical insights while also delivering plan data to providers directly at the point of care. This real-time access to critical member data significantly boosts risk recapture and care gap closure rates.
Value-Based Care Success
Azara's deep analytics provide a granular view of performance at the network, practice, and provider levels, enabling data-driven decisions for continuous improvement.

NCQA Data Aggregator Validation
Azara Healthcare was part of the first cohort organizations which earned Certified Data Stream status in 2021 for NCQA’s Data Aggregator Validation Program - the highest level of certification offered by the National Committee for Quality Assurance (NCQA).
Validated data flows promote trust in aggregated clinical data. They support adoption of value-based contracting by making many of its core features more workable. This also eases the quality measurement load - validated data streams are uniquely accepted as standard supplemental data in HEDIS® audits. This means no primary source verification is required for HEDIS reporting when health plans report data from validated sources.
Validated data flows are an important, early step on the pathway to a digital measurement ecosystem.
Frequently Asked Questions
What’s the best way to identify missed opportunities in Value-Based Care programs?
Missed opportunities are often found by analyzing quality gaps, utilization patterns, and attribution data. Azara helps organizations identify where interventions can improve performance and maximize shared savings.
How can clinical teams use VBC reporting to improve patient outcomes?
VBC reporting translates performance data into actionable insights for clinical teams. Azara provides timely reports that help teams focus on patients who will benefit most from intervention.
How does payer-provider collaboration help with Value-Based Care success?
Collaboration improves data sharing, alignment on goals, and care coordination. Azara supports payer-provider collaboration by enabling shared visibility into performance, quality, and utilization metrics.
What should I do if I don’t have access to payer data?
Even without payer data, organizations can make progress using clinical and utilization data. Azara helps organizations optimize performance with the data they have while supporting future integration of payer information.
Additional Resources
MARKET REPORT
Download our findings report to learn what is slowing VBC progress for providers and health plans
LEARNING SERIES
Subscribe to the weekly Learning Series: The Six Essential Elements for Value-Based Care Success
SUCCESS STORY
Regional Louisiana health plan partners with Azara Healthcare on chronic disease management for value-based innovation in primary care



